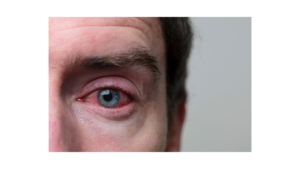
Have your eyes been itchy and driving you crazy? It might not be what you think it is. Allergic conjunctivitis with hay fever, dry eye, pink eye or blepharitis could lead to wrong treatment and side effects.
With an estimated 50 million white blood “mast” cells, the eye can sense irritants and release histamine and other substances to defeat the irritants. Histamine stimulates eye nerve endings which irritates the eyes causing the itch.
Approximately 50 million people in the U.S. have allergies. Some are allergic to environmental triggers but the majority experience symptoms when grass, pollens and mold are in the air. Common allergens include pollen, dust mites, ragweed, mold, pet dander, perfumes, smoke and some fragrances or cosmetic ingredients.
When allergies target the eyes, the condition can be miserable. Eye conjunctivitis may get treated as part of a nasal allergy or it can be mistaken for other serious conditions like infectious conjunctivitis also known as pink eye, dry eye disease, blepharitis (inflammation of the eyelids), herpes virus or keratitis (corneal ulcer).
Making these distinctions is critical to ensuring the proper treatment is diagnosed, to quickly reduce the symptoms and reduce the potential risk of harm to the eyes. The American College of Allergy, Asthma and Immunology (ACAAI) warns that extended use of some nasal allergy medications can leave allergic eyes drier and even more irritated.
Usually if the eyes are itchy and watery, it’s probably an allergy with intense itching with tearing and redness.
Seasonal Allergic Conjunctivitis
Most of the eye allergies in the U.S. are seasonal conjunctivitis occurring in the spring, summer and fall. Symptoms include dark under the eye circles, light sensitivity and puffy eyelids.
Perennial Allergic Conjunctivitis
This condition is where eye allergies occur year-round but commonly caused by household/workplace irritants, dust mites, mold and pet dander. The symptoms are the same as seasonal conjunctivitis but usually less severe.
Vernal Keratoconjunctivitis
This year-round condition and worsen during pollen seasons and targets boys, young men, and people with asthma or eczema. Symptoms include the feeling of something in your eye and light sensitivity.
Atopic Keratoconjunctivitis
Another year-round atopic (sensitive to allergens) keratoconjunctivitis, this strikes older men who have allergic dermatitis (an immune reaction in the skin). Symptoms are eye burning and a thick mucus that accumulates on eyelids overnight.
Contact Allergic Conjunctivitis
Direct contact with potential allergens such as eye drops with preservatives can lead to this reaction. Symptoms can also cause discomfort wearing contact lenses and mucus discharge.
Giant Papillary Conjunctivitis
This severe condition leads to fluid sacs (papules) forming in the upper eyelid lining. Doctors can see them by turning the lids inside out. Other symptoms include blurry vision from mucus discharge, foreign body sensation, discomfort wearing contacts and a sense that contacts are moving, puffy or droopy eyelids.
What else could it be other than an eye allergy?
Pain in the eye or diminished vision are serious symptoms not typical for allergies. Dry Eye Disease (DED) allergy and DED are very similar. Pink eye causes red, painful eyes indicating infection of inflamed conjunctiva. Pink eye is very contagious and usually begins in one eye and generates a sticky secretion that coats the lashes. A swollen lymph not by the ear may also appear.
Pollen clogged tear grands can resemble blepharitis, a disorder of the eyelid’s oil producing glands. It can almost always be infectious and symptoms include irritation, redness, flaky eyelid skin and crusted lashes.
Karatitis is the inflammation of the cornea, and symptoms include redness, pain, watering, blurry or decreased vision and rarely itchiness. Herpes eye disease can lead to pain, tearing, redness, light sensitivity, and a skin rash or sore near the eye. Observation or special blood tests can confirm this disease.
Other itchy conditions include contact dermatitis, atopic eczema and psoriasis all have itching on the eyelid or the skin around the eye.
Prevention
- Avoid a known allergen
- Protect eyes with sunglasses, visored hats and swimming goggles
- Wash hands when coming indoors (especially after handling animals)
- Wash your face to clean off allergens
- Soothe eyes with a cold compress
- Try preservative free tear substitutes
- Consider mite-proof bedding
- Wash sheets and blankets in hot water weekly
- Check for and eliminate mold by regularly cleaning the areas of your home where moisture may accumulate (base of the toilets, closets, mudrooms, HVAC filers, water filters, windowsills and gutters
- Use air conditioning in your car and in your home
- Leave your shoes at the door
Avoidance
- Eye drops with herbal extracts
- Eye products using preservatives
- Window fans that draw in allergens
- Indoor humidity exceeding 50 to 50 percent to discourage mold
- Dry dusting or sweeping floors and spreading allergens
- Wearing contact lenses too long
- Rubbing eyes
If you think you might have an eye allergy, discuss this with your OAAC provider. There are many types of drugs and treatments available. Your OAAC allergist can find the right mix of medication and treatment to defeat the eye allergy itch.
